Natural IVF: A Gentler Path for Women Over 35
- Feb 22
- 12 min read
Updated: Mar 18

Finding options that respect your body’s rhythm can feel out of reach when you face diminished ovarian reserve. Many women over 35 worry that their fertility choices are limited or that Natural IVF is somehow less effective than conventional methods. In truth, this gentler approach works with your natural cycle, offering a path with fewer medications and near-zero risk of ovarian hyperstimulation syndrome. Unpacking common misconceptions about Natural IVF reveals why it could be the personalized solution to support your journey.
Table of Contents
Key Takeaways
Point | Details |
Natural IVF Utilizes the Body’s Cycle | Unlike conventional IVF, Natural IVF works with your body’s natural hormonal rhythm, retrieving one mature egg without hormonal stimulation. |
Quality Over Quantity Matters | Natural IVF emphasizes obtaining a single quality egg, often more valuable for women over 35 than multiple lower-quality eggs. |
Safer Alternative | Natural IVF has a significantly lower risk of ovarian hyperstimulation syndrome and fewer hormone-related side effects compared to conventional methods. |
Cost-Effective Option | Natural IVF is generally 40-50% less expensive than conventional IVF, offering a more affordable choice for many women. |
Natural IVF Defined and Common Misconceptions
Natural IVF is fundamentally different from what you might imagine. It’s a cycle using your body’s own hormonal rhythm without stimulation medications.
Unlike conventional IVF, which uses gonadotropin injections to trigger multiple egg development, natural IVF works with your body’s single monthly egg. This approach retrieves one mature egg during your natural menstrual cycle, eliminating the need for hormone stimulation.
Here’s what actually happens:
Your body releases one egg naturally (monofollicular development)
Doctors monitor this single follicle through ultrasound and blood work
The egg is retrieved at the optimal time
Fertilization and embryo transfer proceed as with conventional IVF
No injectable hormones required
The beauty here? Your body does what it’s designed to do. You’re simply working with your natural cycle rather than overriding it.
The Misconceptions Holding You Back
Misconception #1: Natural IVF is less effective. This needs clarification. While natural cycle IVF is associated with lower pregnancy rates per cycle, that’s partly because you’re attempting fewer retrievals—not because the procedure itself fails. For women over 35 with diminished ovarian reserve, one quality egg is often more valuable than multiple poor-quality eggs.
Misconception #2: You need stimulation to get results. False. Many women over 35 actually experience better outcomes with natural IVF because it focuses on quality over quantity.
Misconception #3: It’s risky. The opposite is true. Natural cycle IVF has near-zero risk of ovarian hyperstimulation syndrome, making it significantly safer than conventional approaches for your body.
Misconception #4: There’s a high cancellation rate. Yes, cycles can be canceled if ovulation occurs before retrieval. But this isn’t failure—it’s your body working normally.
Natural IVF isn’t a competing treatment to conventional IVF; it’s a complementary option designed for specific patient populations and goals.
For women over 35, understanding these distinctions matters. You’re not choosing an inferior option. You’re choosing an approach tailored to your reproductive reality. When exploring types of IVF procedures available, natural IVF deserves serious consideration as part of your personalized treatment plan.
Pro tip: Ask your fertility specialist whether a natural IVF cycle makes sense for your specific ovarian reserve status and egg quality—the answer might surprise you.
How Natural IVF Works Step by Step
Natural IVF follows a carefully timed sequence that respects your body’s biological rhythm. Understanding each phase helps you know what to expect and prepares you mentally for the process.
The timeline typically spans 10-14 days from monitoring start to embryo transfer. This is shorter than conventional IVF cycles, reducing stress and physical strain on your system.
Step 1: Baseline Monitoring
You’ll begin with an ultrasound and blood work on day 3 of your menstrual cycle. This establishes your baseline hormone levels and confirms your ovaries are ready.
Your doctor checks:
Follicle-stimulating hormone (FSH) levels
Estrogen baseline
Antral follicle count
Uterine lining thickness
This step ensures you’re a good candidate for that particular cycle. Some cycles get canceled here if hormone levels aren’t optimal.
Step 2: Natural Follicle Development Monitoring
Starting around day 8-10, you return for frequent monitoring. Your single dominant follicle develops naturally without injectable hormones.
Monitoring includes:
Ultrasounds every 1-2 days
Blood work to track estrogen rise
Precise measurement of follicle growth
Observation of uterine lining development
Your doctor watches for the follicle to reach 17-18 millimeters. This is the sweet spot for maturity without premature ovulation.
Step 3: Trigger Injection
Once your follicle reaches optimal size, you receive a single hCG trigger injection (human chorionic gonadotropin). This mimics the natural LH surge that triggers ovulation.
Timing is critical. The injection occurs roughly 35-37 hours before egg retrieval. Your doctor calculates this precisely to catch the egg at peak maturity.
Step 4: Egg Retrieval
Retrieval happens under light sedation. A thin needle passes through your vaginal wall into the follicle, gently extracting the mature egg.
The entire procedure takes 15-20 minutes. You go home the same day, though you’ll feel groggy from sedation for a few hours.
Step 5: Fertilization and Culture
Your single egg is combined with sperm (partner’s or donor) in the laboratory. The embryo develops for 3-5 days in a controlled environment.
Your embryologist monitors development daily. By day 3 or day 5, you’ll know if fertilization was successful and how the embryo progresses.
Step 6: Embryo Transfer
A quality embryo is transferred into your uterus using a thin catheter. This is a simple, quick procedure requiring no sedation.
You return home immediately after. The embryo naturally implants over the next 6-12 days.
Natural IVF’s strength lies in its focus on quality—one excellent embryo beats multiple mediocre ones.
The entire process prioritizes your biological rhythm rather than forcing artificial stimulation. When you’re considering ways to increase IVF success naturally, understanding this step-by-step process reveals why natural cycles can work exceptionally well for women over 35.
Pro tip: Track your cycle patterns for three months before starting natural IVF—knowing your ovulation timeline helps your doctor predict trigger timing more accurately, reducing cycle cancellations.
Types of Natural and Modified IVF Cycles
Not all natural IVF approaches are identical. The spectrum ranges from completely unstimulated cycles to mildly enhanced versions that give you more control over timing.
Understanding these variations helps you and your doctor choose what fits your body, goals, and risk tolerance. Each cycle type addresses different challenges women over 35 face.
Natural Cycle IVF (NC-IVF)
Natural Cycle IVF relies entirely on your body’s hormone production. Zero stimulation medications. Your single egg develops on its own timeline.
What happens:
No injectable gonadotropins
No oral hormone medications
Monitoring tracks your natural LH surge
One mature egg retrieved per cycle
Minimal hormone-related side effects
This approach works best if your cycle is regular and predictable. It’s ideal for women concerned about hormone exposure or those with diminished ovarian reserve who don’t respond well to stimulation.
Modified Natural Cycle IVF (MNC-IVF)
Modified Natural Cycle IVF adds minimal medications to prevent your egg from ovulating before retrieval. You still develop one dominant follicle naturally, but the timing becomes more controllable.
Medications used:
GnRH agonists or antagonists (prevent premature ovulation)
Low-dose oral contraceptives (stabilize your cycle)
Minimal hormone exposure compared to full stimulation
Modified Natural Cycle IVF shows enhanced activation of pathways supportive of implantation compared to fully stimulated cycles. This means better embryo quality despite the gentle approach.
Most women prefer this option. You get natural egg development plus protection against cycle loss from premature ovulation. The medication dose is minimal—far lower than conventional IVF.
Mild Stimulation IVF
Mild Stimulation IVF uses low-dose gonadotropins to stimulate 2-5 eggs instead of just one. It’s gentler than full stimulation but produces multiple eggs for selection.
Benefits for women over 35:
More eggs retrieved (increases chances of viable embryos)
Lower medication doses than conventional IVF
Fewer monitoring appointments than full stimulation
Reduced risk of ovarian hyperstimulation
Shorter hormone exposure period
This bridges the gap between natural IVF’s single-egg approach and conventional IVF’s multiple-egg retrieval.
The choice between natural, modified, and mild stimulation cycles isn’t about one being “better”—it’s about matching the approach to your specific reproductive situation.
Each cycle type differs biologically and clinically, justifying tailored clinical use based on your needs and risk profile. Women over 35 with diminished ovarian reserve often find modified natural IVF offers the ideal balance.
Here’s how natural, modified natural, and mild stimulation IVF cycles differ:
IVF Cycle Type | Medication Use | Egg Retrieval Focus | Ideal Candidate |
Natural | No hormones | One top-quality egg | Regular cycles, sensitive to meds |
Modified Natural | Minimal—prevents early ovulation | One mature egg | Unpredictable ovulation, prior cycle cancellation |
Mild Stimulation | Low gonadotropins | 2-5 eggs per cycle | Seeks more embryos, moderate ovarian reserve |
Pro tip: Ask your fertility doctor which cycle type suits your FSH levels, age, and previous IVF response—your ideal option depends on these individual factors, not on what worked for someone else.
Who Should Consider Natural IVF Options
Natural IVF isn’t for everyone, but if you fit certain criteria, it might be your ideal path forward. The question isn’t whether natural IVF works—it’s whether it matches your specific reproductive profile.
You’re a candidate if you recognize yourself in these situations. Let’s break down who benefits most from this gentler approach.
Women at Risk of Ovarian Hyperstimulation
If you’ve experienced ovarian hyperstimulation syndrome (OHSS) before, or your doctor warned you about the risk, natural IVF eliminates this concern entirely. Without hormone injections, OHSS simply cannot occur.
OHSS causes:
Severe bloating and abdominal pain
Nausea and vomiting
Rapid weight gain (2+ pounds daily)
Shortness of breath in severe cases
Hospital admission in extreme situations
Women with polycystic ovary syndrome (PCOS) or those who are young with high antral follicle counts face the highest OHSS risk. If this describes you, natural IVF provides peace of mind alongside effective treatment.
Poor Responders to Gonadotropins
Your body might not cooperate with stimulation medications. Some women over 35 have diminished ovarian reserve that doesn’t respond well to hormone injections—you produce few or no mature eggs despite high medication doses.
This is incredibly frustrating. You pay, you inject, you monitor, and nothing happens. Women seeking a gentler approach with fewer medications benefit from natural IVF’s reduced hormone exposure, especially when previous stimulation cycles yielded disappointing results.
Natural IVF focuses on your body’s actual capability rather than forcing it into an unnatural response.
Women with Diminished Ovarian Reserve
If your FSH is elevated and your antral follicle count is low, stimulation might not offer much advantage. You’re already producing fewer eggs naturally.
Here’s the logic: conventional IVF might retrieve 3-5 poor-quality eggs from your diminished reserve. Natural IVF retrieves 1 potentially excellent egg. Quality beats quantity when your reserve is limited.
Those Seeking Fewer Physical and Emotional Burdens
IVF demands sacrifice—time off work, daily injections, frequent appointments, emotional ups and downs. Some women over 35 simply want a less invasive path.
You might qualify for natural IVF if:
You prefer avoiding hormone injections
You want fewer monitoring appointments
You’re concerned about long-term hormone exposure
You need flexibility with work or family schedules
You’ve experienced emotional stress from previous cycles
Natural IVF is ideal for women who ask: “What if I just worked with my body instead of against it?”
When developing your treatment plan, discussing best practices for IVF in 2026 specifically designed for women over 35 helps you understand whether natural or modified cycles align with your goals.
Pro tip: Request detailed blood work and ultrasound analysis before deciding on any IVF approach—your FSH levels, ovarian volume, and previous cycle response determine which option gives you the best statistical outcome.
Risks, Costs, and Comparison With Conventional IVF
Natural IVF carries different tradeoffs than conventional IVF. Understanding the risks, expenses, and outcomes helps you make an informed choice aligned with your finances and health priorities.
Neither approach is universally “better.” They’re different tools for different situations.
Risks: Natural IVF vs. Conventional IVF
Natural IVF risks:
Cycle cancellation (10-20% of cycles) if ovulation occurs before retrieval
Single egg retrieval means no backup if fertilization fails
Slightly lower per-cycle pregnancy rates than conventional IVF
Minimal hormone-related side effects
Zero risk of ovarian hyperstimulation
No multiple pregnancy risk
Conventional IVF risks:
Ovarian hyperstimulation syndrome (OHSS) in 1-3% of cycles (mild to severe)
Higher multiple pregnancy rates (twins, triplets)
Hormone-related side effects (headaches, mood changes, bloating)
Blood clots in rare cases
Infection during egg retrieval (extremely rare, <0.1%)
For women over 35, the conventional IVF risk profile matters more if you have PCOS or high ovarian reserve. Natural IVF’s main risk is cycle loss from poor timing, not medical complications.
Cost Comparison
Conventional IVF typically costs $12,000-$15,000 per cycle in the United States. Natural IVF runs $4,000-$8,000 per cycle—roughly 40-50% less.
But here’s what matters more: total cost per live birth. Natural and mild IVF cycles reduce medication costs and risks of multiple pregnancies, but often have lower per-cycle pregnancy rates.
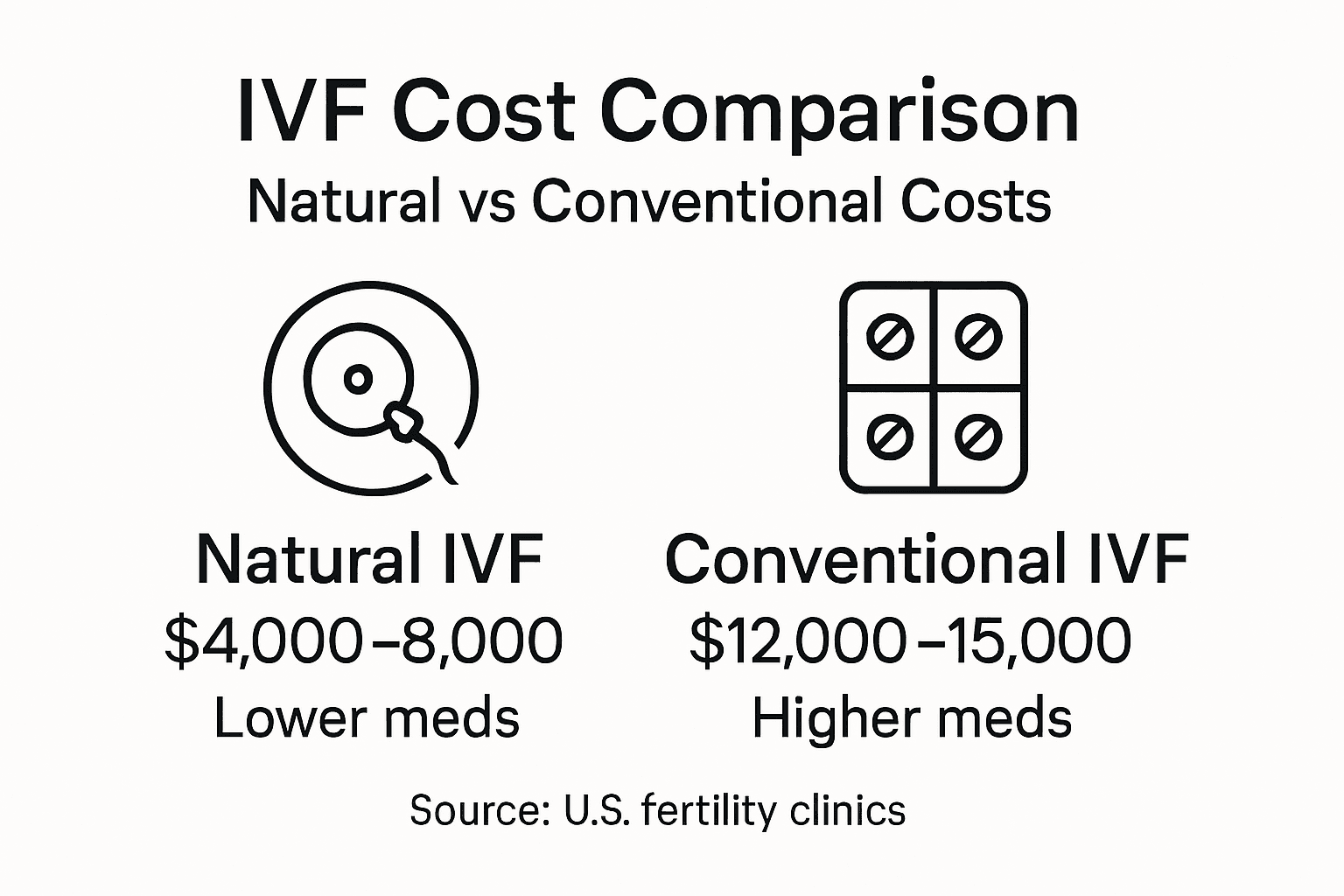
This means:
Compare the most important financial and medical tradeoffs between natural and conventional IVF:
Aspect | Natural IVF | Conventional IVF |
Per-cycle Cost | $4,000–$8,000 | $12,000–$15,000 |
Multiple Pregnancy Risk | Nearly zero | Increased (twins, triplets) |
OHSS Risk | None | Up to 3% of cycles |
Medication Use | Minimal or none | Frequent injections |
Natural IVF: 2-3 cycles might equal one conventional cycle cost-wise
Conventional IVF: One cycle costs more but produces more eggs
You might need multiple natural cycles versus one conventional cycle
Cost factors to consider:
Medication expenses (conventional costs significantly more)
Monitoring appointment frequency (conventional requires more visits)
Egg freezing options (varies by fertility center)
Insurance coverage (rarely covers either, varies by plan)
Travel expenses (if seeking specialized natural IVF providers)
Success Rates and Cumulative Outcomes
Conventional IVF shows higher single-cycle pregnancy rates: 40-50% for women under 35, declining to 10-15% by age 43.
Natural IVF shows lower single-cycle rates: 15-25% depending on your age and egg quality. But cumulative success across multiple cycles can be comparable or better when you account for fewer side effects and cost savings.
The question isn’t which cycle type has the highest per-cycle pregnancy rate—it’s which gives you the best outcome at the price you can afford.
Cost-benefit assessments should consider cumulative live birth rates across multiple cycles rather than comparing single-cycle statistics. A woman doing three natural IVF cycles might achieve similar outcomes to one conventional cycle at half the total cost.
Pro tip: Request a personalized cost analysis from your fertility clinic that projects cumulative outcomes over 3-4 cycles—this reveals your true financial and biological investment, not just single-cycle pricing.
Discover a Personalized and Gentler IVF Approach for Women Over 35
If you are concerned about the physical and emotional challenges of conventional IVF or have experienced low ovarian response or heightened risks from stimulation medications natural IVF offers a compassionate and tailored alternative. This method respects your body’s rhythm by focusing on quality over quantity and greatly reduces risks like ovarian hyperstimulation syndrome. Women over 35 with diminished ovarian reserve or those seeking fewer hormone-related side effects often find renewed hope with natural or modified natural IVF cycles.
At Rejuvenating Fertility Center our expert team led by Dr. Zaher Merhi specializes in designing innovative fertility solutions that match your unique hormonal profile and reproductive goals. Explore our comprehensive services that include specialized IVF options and advanced therapies to support your journey. Don’t wait to find a treatment plan that works gently yet effectively. Visit our main website now to book your personalized consultation and start embracing a fertility path aligned with your body’s natural strengths.
Learn more about the types of IVF procedures available and how we ensure the best outcomes for women over 35. Your compassionate care and success story begin today.
Frequently Asked Questions
What is Natural IVF and how does it differ from conventional IVF?
Natural IVF is a fertility treatment that utilizes your body’s natural hormonal rhythm to retrieve a single mature egg without the use of stimulant medications. Unlike conventional IVF, which involves hormone injections to develop multiple eggs, Natural IVF focuses on one egg that develops in your natural menstrual cycle.
What are the advantages of choosing Natural IVF for women over 35?
Natural IVF offers several benefits, including reduced risk of ovarian hyperstimulation syndrome (OHSS), fewer medications, and a focus on retrieving high-quality eggs. It can also be less emotionally and physically taxing due to fewer appointments and injections, making it a gentler approach for women over 35.
Are the success rates of Natural IVF lower than those of conventional IVF?
While Natural IVF may have lower per-cycle pregnancy rates (15-25% depending on age and egg quality), it’s important to consider cumulative success rates across multiple cycles. Women over 35 with diminished ovarian reserve can still achieve favorable outcomes with natural cycles by focusing on quality over quantity.
Who should consider Natural IVF as an option?
Natural IVF is ideal for women over 35 who are at risk of ovarian hyperstimulation, have poor responses to stimulation medications, have diminished ovarian reserve, or seek a less invasive treatment approach with fewer hormones and emotional burdens.
Recommended


Comments